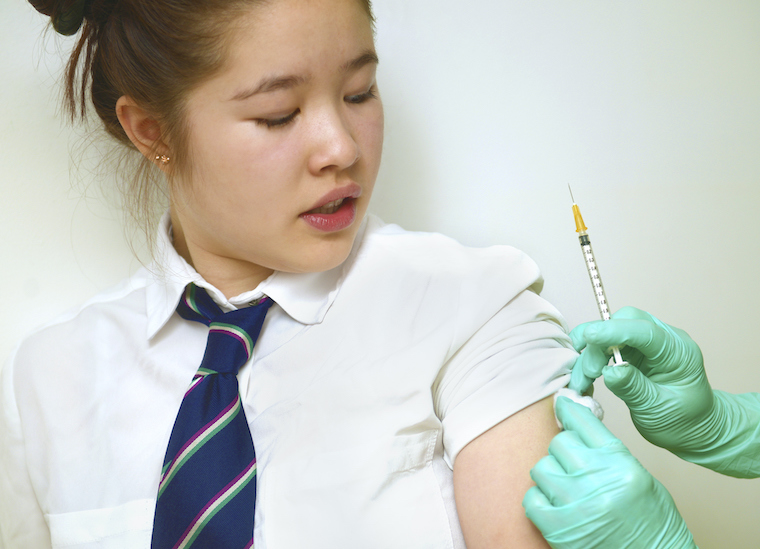
Getting the HPV vaccine can prevent several forms of cancer.
A study has identified the Virginians least likely to know that there is a potentially lifesaving vaccine available for human papillomavirus (HPV), which is responsible for up to 10% of all cancers.
More than a quarter of respondents to a survey of state residents had not heard of the vaccine. Those least likely to be aware include males, urban residents and people who reported lower incomes. Those most likely to know of the vaccine include part-time workers, younger people and those with higher education.
“Our study found particular knowledge disparities by sex, age, rurality, income and education in our state,” said researcher Rajesh Balkrishnan, PhD, of the School of Medicine’s Department of Public Health Sciences and UVA Cancer Center. “We need to elucidate these barriers to knowledge, which could inform new statewide policies about ensuring the uptake of this important vaccine.”
About HPV
HPV is the most common sexually transmitted disease in the United States, infecting 18 million Americans each year. It is estimated to cause more than 90% of cervical and anal cancers and 75% of vaginal cancers, as well as substantial percentages of cancers of the penis, mouth and throat.
More than 4,000 American women are expected to die this year of cervical cancer alone.
To gauge public awareness of the HPV vaccine, UVA Cancer Center and Virginia Commonwealth University’s Massey Cancer Center surveyed almost 1,500 people across the areas where most of their patients live. This includes most of the state. The researchers aimed to determine whether there were associations between vaccine awareness and respondents’ sex, race, age, place of residence, education level, income, job status and health insurance.
The key predictors of vaccine awareness they identified include sex, education and rural vs. urban residence. “Being male, living in an urban area, or having an income from $35,000 to $49,999 relative to an income of $50,000 to $99,999 substantially decreased the odds that an individual has knowledge of the HPV vaccine,” the researchers write in a scientific paper outlining their findings.
People with part-time jobs were more likely to be aware of the vaccine, possibly because this group includes many college students, the researchers speculate. Younger people and those with more education were more likely to know of the vaccine in general.
Awareness, however, is just one component of convincing the public of the value of the vaccine, the research team notes. In 2016, only 41.1% of Virginia girls ages 13 to 17 were up-to-date on their HPV vaccine; that percentage was even lower, 37.4%, for boys.
“Knowledge is only the first step to increasing HPV vaccination rates,” the researchers write. “Although this survey indicated that 72.26% of participants have heard of the HPV vaccine, this does not translate to intention to receive it or to vaccinate their children and family members.”
The researchers say further research is needed to better understand HPV vaccine hesitancy across Virginia.
“Increased knowledge and use of the HPV vaccine is crucial in reducing the spread of the virus and associated cancer risk in Virginia,” Balkrishnan said. “And knowledge is only the first step to increasing HPV vaccination rates. We need policies to prioritize the uptake of this vaccine in all Virginia teens.”
Findings Published
The researchers have published their findings in the Virginia Journal of Public Health. The research team consisted of Mythili Vigneshwar, Sunny Jung Kim,Carrie A. Miller, Bernard Fuemmeler and Balkrishnan.
The work was supported by the National Cancer Institute, grantsP30CA044579-27S5 (UVA) and P30 CA016059-3.
To keep up with the latest medical research news from UVA, subscribe to the Making of Medicine blog.
MORE FROM BALKRISHNAN: Colorectal cancer screening lagging among rural women.



